Other Central Hemodynamic Parameters
The first step to evaluate the cardiovascular status of the patient is to look over the central hemodynamic parameters. Assessment of these parameters give us an overall view about the function of the heart and main vessels as the key organs of human body. Analysis of these parameters estimate the risk of future cardiovascular events such as hypertension, atherosclerosis and its consequences like stroke, coronary artery diseases etc.
The essential parameters like pulse wave velocity and central systolic blood pressure have already been discussed in details as main parameters measured by Arteriograph. Here we explain other informative parameters which along the main indicators, provide a clear image about cardiovascular system.
Aortic Pulse Pressure (PPao)
At the end of each systole in cardiac cycle, after isovolumetric contraction, the blood will be pumped through aortic valve to supply the systems. This will be followed by an isovolumetric relaxation and thus inflow. The time between two mentioned stages is called ejection duration. In the other hand the period of blood flow through aortic and pulmonary valves.
Pulse pressure is calculated as difference between the central systolic and diastolic pressure. High pulse pressure is an important risk factor for cardiovascular disease and low pulse pressure could be a sign for insufficient preload. PPao is considered to be normal under 50 mmHg.
PPao= SBPao – DBPao
Ejection Duration
Aortic pulse pressure is determined from interaction of different circulatory events: cardiac output, arterial compliance, and peripheral resistance. It is not only reflects generated force by the heart but also the changes in volume according to the alteration of the aortic transmural pressure. Therefore, the higher the pulse pressure the less is the aortic compliance. It is also directly proportional to stroke volume.
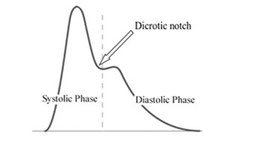
ED’s Normal value is influenced by the heart rate and is measured from blood pressure tracings as the interval from end diastole to the dicrotic notch.
ED = time interval between the beginning of the heart cycle until the dicrotic notch
Return Time
Return time of the aortic pulse wave is the time between the spikes of the direct and reflected pressure waves. It reflects the characteristics of the aortic wall. The stiffer the aortic wall, the lower the RT is. RT is normal above 120 msec.
RT= time between P1 and P2
Diastolic Reflection Area
The left coronary artery practically is perfused only in the diastole. Thus, the filling conditions of the left coronary artery during diastole is in a strong relation to the oxygenation of the left ventricle.
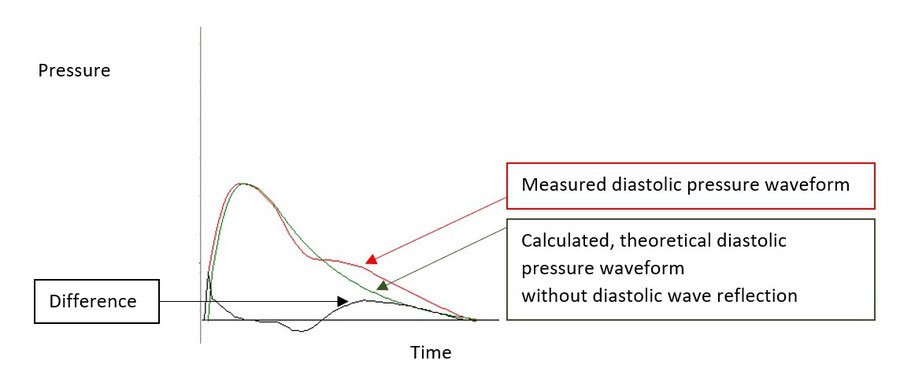
The DRA provides information on the quality of the left coronary filling conditions during diastole. This parameter is partly based on the duration of the diastole, and on the other hand on the area difference, calculated without wave reflection in the diastole (theoretical, mathematically calculated) and the actual recorded pressure at the diastole with diastolic wave reflection. I.e., the theoretical diastolic pulse pressure waveform without reflection is subtracted from the recorded diastolic pulse pressure waveform. The DRA is a dimensionless parameter.
Systolic/Diastolic Area Index
Systolic area index (SAI), DAI = diastolic area index. Pressurising the cuff to the diastolic blood pressure volumetric signals can be obtained. The area under the curve is taken as 100%, and then it is divided into systolic (SAI) and diastolic (DAI) area and expressed as the percentage of the total (100%). In normal, resting situation with normal heart rate the SAI used to be less than 50% and the DAI more than 50%. The lower third of the DAI is under 46%, which could be considered abnormally low.
Systolic Blood Pressure
Systolic blood pressure is the amount of force applied to the arteries by contraction of heart, thus forcing the distinct amount of blood to the arteries. This pressure is commonly seen in every blood pressure measurement as the top number. It can be measured through different methods of manometry. Ideal range of Systolic blood pressure is between 90-120 mmHg.
Diastolic Blood Pressure
Diastolic Blood Pressure refers to the pressure applies to the wall of arteries due to their own elastic characteristic upon passage of the blood. In the other word it is the pressure measured during diastole or relaxation stage of the heart. Same as systolic blood pressure it can be measured using manometric methods and it is always seen as the number in the bottom. Below 80 mmHg is considered as normal value.
Mean Arterial Pressure
The mean arterial pressure is the average pressure throughout the cardiac cycle. Because the systole is shorter than diastole, the mean pressure is slightly less than the value halfway between systolic and diastolic pressure. As an approximation, mean pressure equals the plus one third of pulse pressure. The value between 70 and 100 mmHg is usually considered to be normal.
MAP = DP + 1/3(PP)
Heart Rate
Heart rate, or pulse, is the number of times the heart beats per minute. The measurement needs a stethoscope or any blood pressure measuring devices. The normal range for adults is between 60-100 beats per minute.
In evaluating a patient's health with Arteriograph, Prof. Miklós Illyés introduced some central hemodynamic parameters for the first time. These consist of Diastolic Reflection Area and Systolic/Diastolic Area Index. It's important to mention that these parameters, now referred to as fitness parameters, are still being explored and need further investigation.